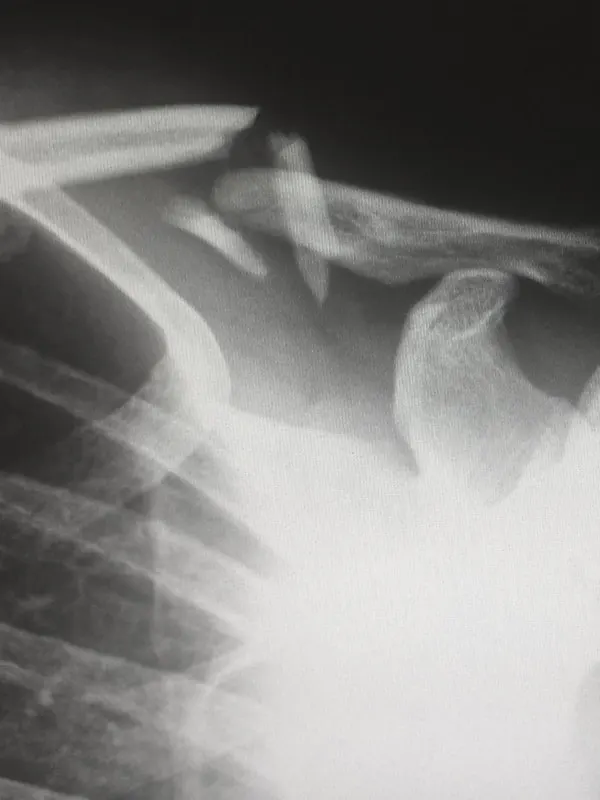
Patients skip the injection
they can't see the reason for.
A patient with 'broad-based disc protrusion at L4-L5 with moderate foraminal stenosis' nods politely, cancels the epidural, and is back in your office in six weeks worse than when they left. A visual report turns a vague diagnosis into a reason they show up. It also turns a hedged report into a prior-auth submission that carries its own argument.
The gap between diagnosis and follow-through.
Patients cancel the injection they don't understand.
Epidurals, facet blocks, nerve blocks: compliance depends entirely on the patient believing in the anatomy.
Patients show up when they see the compression.
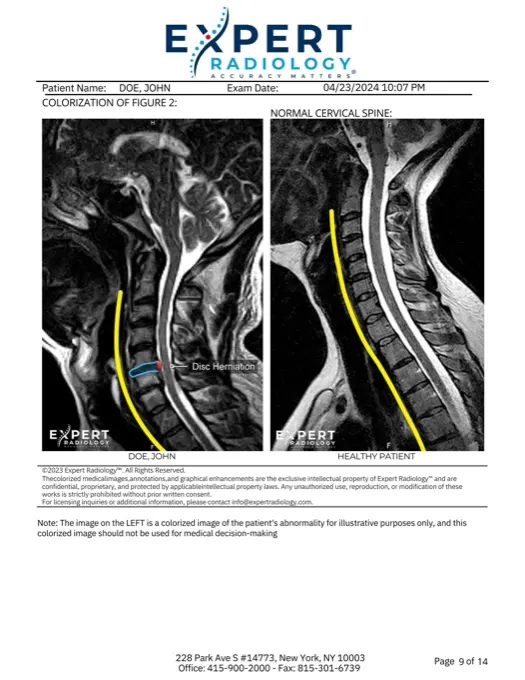
A colorized nerve-root image at the target level turns an abstract procedure into a visible intervention.
Prior auth rejects the hedged report.
"May represent," "cannot exclude," "correlate clinically." Every hedge word is a reason a payer says no.
Direct, subspecialist language.
v3™ reports describe what is actually there. Prior-auth submissions carry their own evidence.
Chronic patients drift out of the plan.
Without ongoing visual justification, long-term management gets renegotiated at every visit.
A document they keep.
Visual reports become a reference the patient revisits between injections, therapy, and follow-ups.
This is the image that turns a diagnosis into a decision.
PrecisionPlus v3™ Report
Spine and pain-focused reads paired with colorized key images, custom medical illustrations, and plain-language summaries. One report built for injection compliance, prior authorization support, and patient follow-through.
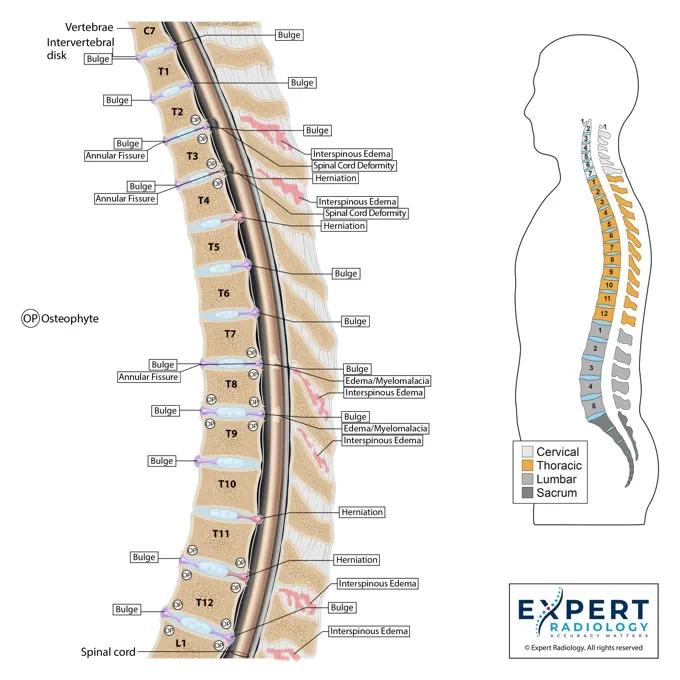
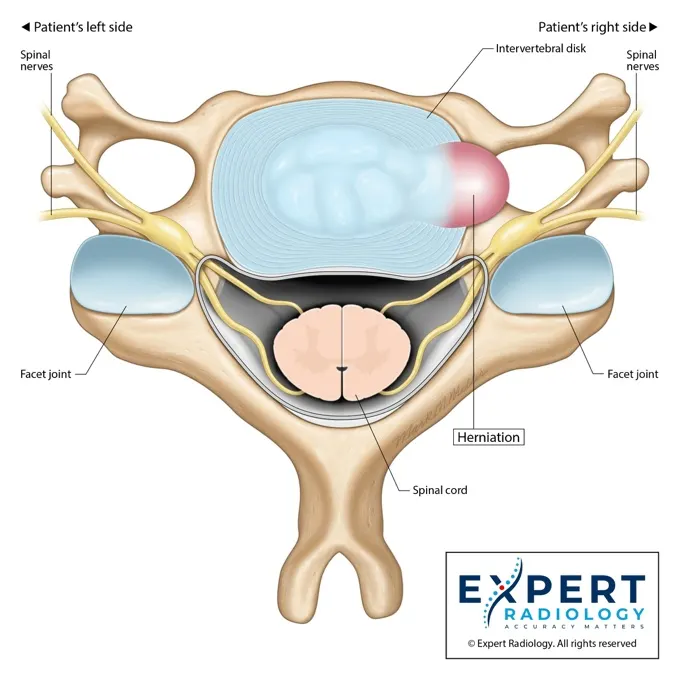
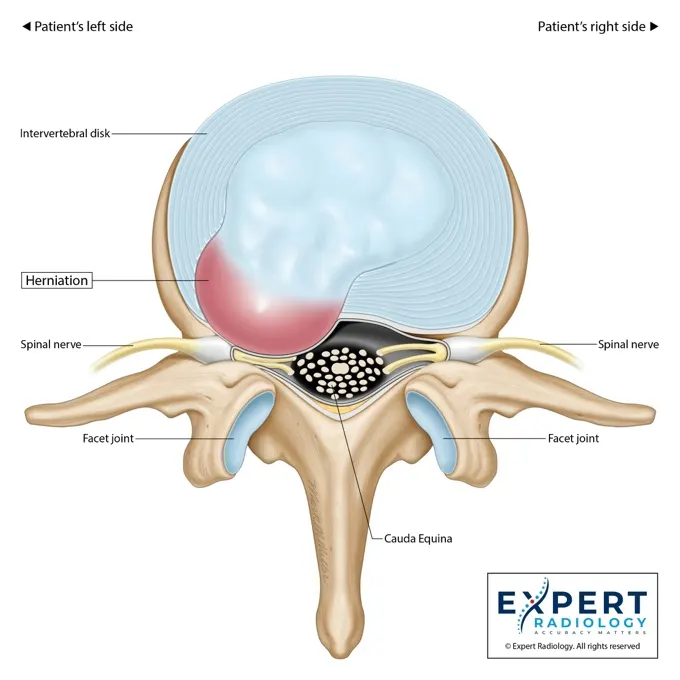

Built for compliance and prior auth.
Visual evidence and direct subspecialty language make treatment rationale easier for patients, referrers, and payers to follow.
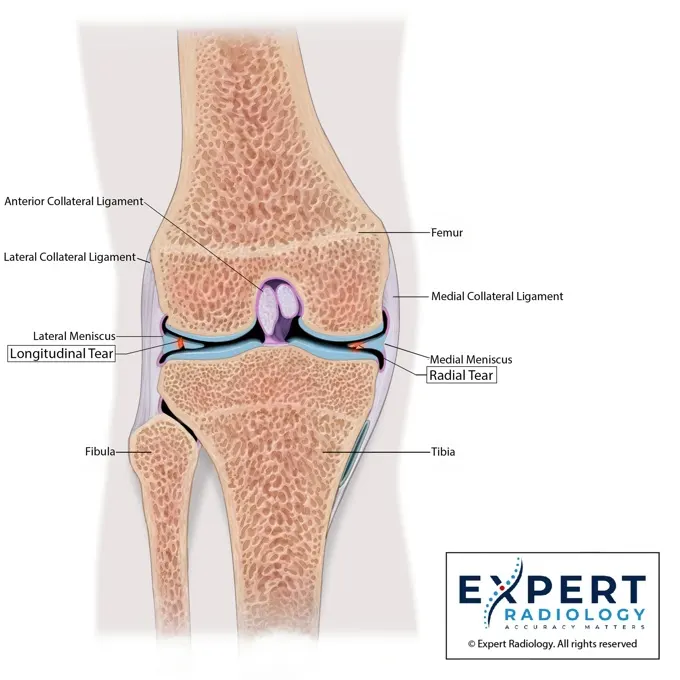
Colorized Key Images
Patients see the nerve compression and show up for the injection.
Plain-Language Summary
Prior-auth submissions carry their own argument.
Subspecialty Read
Neuroradiology and MSK reads that catch nerve-root involvement other readers miss.
How it works for your practice.
Three steps, minimal workflow disruption. Use your existing imaging center or one from our network.
Submit the MRI.
Through the ExRad Portal or your imaging partner.
We deliver a v3™ report.
Subspecialty-focused read, neuroradiology for spine or MSK for joint, with colorized key images and plain-language summary. Status stays visible through delivery.
Use it everywhere.
Patient consults, injection planning, prior-auth submissions, and PI case files, all from the same report.
Common questions from
pain management providers.
Everything you need to know about v3™ reports, injection compliance, and prior authorization.
Yes. v3™ reports use direct, subspecialist language without hedge words. The visual annotations provide the medical-necessity evidence payers require.
Absolutely. Annotated images show exactly where nerve compression, facet degeneration, or disc pathology is occurring. Both the patient and the referring provider see the rationale for the target level.
Same report, dual use. The visual evidence that drives treatment compliance also strengthens demand letters and mediation exhibits.
Turnaround depends on case complexity, clinical priority, current volume, and the agreed workflow. Urgent cases are prioritized appropriately.
See what your patients should be looking at.
Request a sample v3™ report and see the document your patients take home instead of a wall of grayscale and medical jargon.

Attorney's Guide to Radiology Imaging
Everything attorneys need to know about radiology, from ordering the right study to using imaging evidence at trial.